Sciatica
What is it & How to fix it
The term ‘Sciatica’ refers to pain felt in the buttock or leg. It is not so much a diagnosis but more a set of symptoms telling us that something is happening, somewhere along the sciatic nerve pathway.
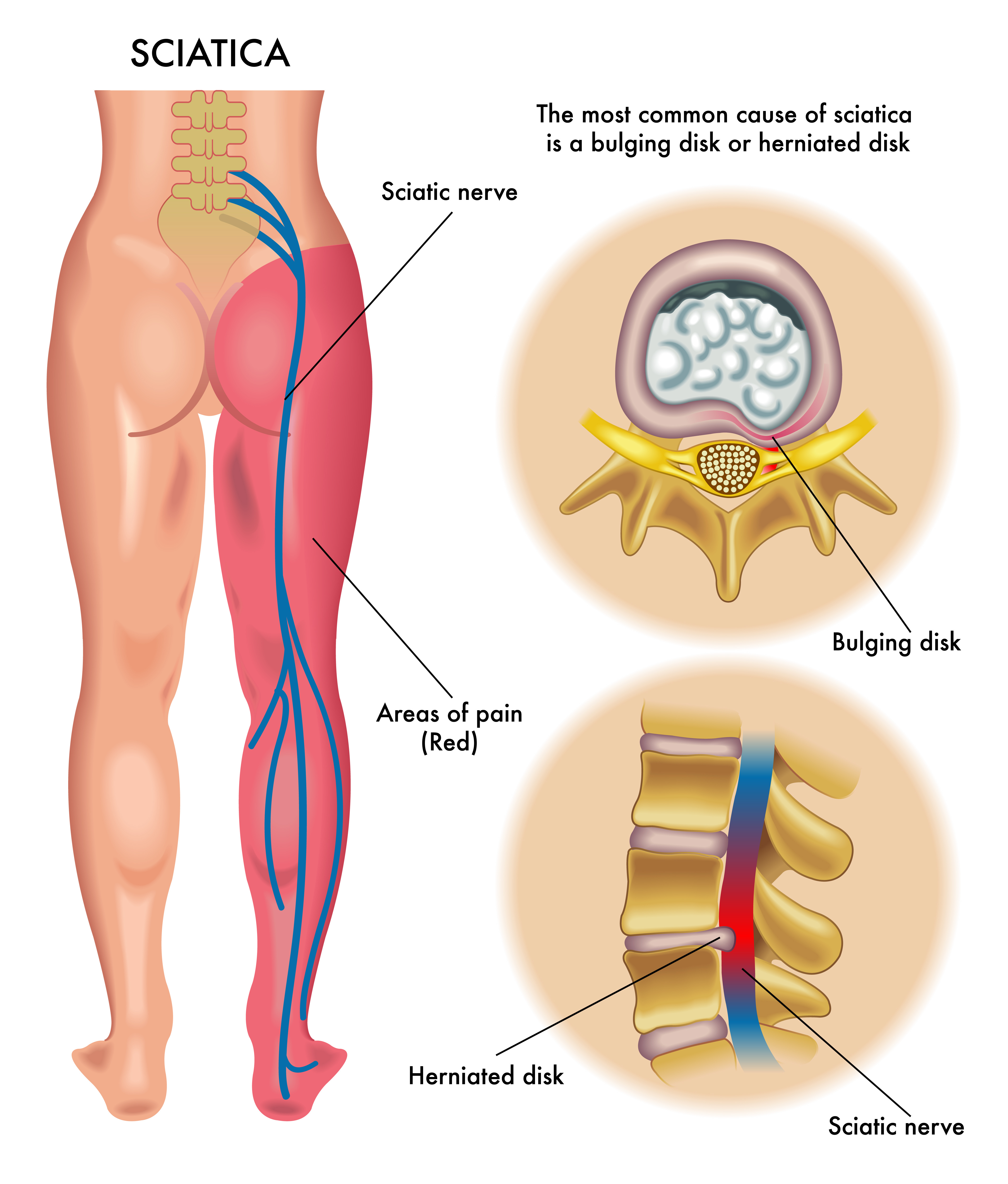
The sciatic nerve runs from the back, through the pelvis and buttock region, down the back of the leg and then into the foot. If there is irritation of this nerve it can cause symptoms in any or all of these regions.
Sciatica can be caused by something compressing or irritating the sciatic nerve or the smaller nerve roots exiting the spinal column. Common causes include a low back disc bulge or prolapse, arthritis of the lumbar spine, and pressure or impingement of the nerve as it passes through the soft tissues in the hip and leg.
Sciatica can also commonly be the result of inflammation anywhere along its pathway, and this is often a major component of acute lumbar disc pathologies. Often disc bulges are no where near big enough to really create pressure on the nerve, but the inflammatory chemicals involved in cleaning up and repairing the disc can still irritate and excite the nerve from some distance away.
People can experience sciatica as an acute event or as an ongoing, persistent condition. In both cases it is vital to understand what the cause is and how the pain is being generated.
In an acute scenario there is usually some sort of initiating event followed by tissue trauma, damage and/or inflammation. As discussed above, a protruding disc can irritate the nerve roots and cause changes in the function of the sciatic nerve. It can be extremely painful and there may be altered sensation and lack of strength in the hip and leg.

In the chronic scenario there are some other factors that need to be identified. In cases where sciatica has persisted for longer than a few months it is unlikely that there will still be physical tissue damage present. Unless you have other substantial health issues that limit your ability to repair and maintain tissue, this tissue should have healed. So, why would it continue to be painful then?
Because, in chronic cases of sciatica the problem is with how the sciatic nerve is behaving rather than how it looks structurally. Simply put, if the nerve functions poorly for more than a few months it can continue to function poorly after the acute injury has healed. So that disc injury you had 1 year ago is no longer the issue – it is no longer ‘a disc prolapse’ – it is the nerve function that needs to be assessed and treated.
This is a very common oversight in the treatment of sciatica. At Melbourne Osteohealth we frequently see people that have ‘old disc injuries’ and ‘nerve compression’ and years after their initial injury they are convinced they will have sciatica forever. If the nerve has not been treated properly it is unlikely the symptoms will resolve. Good thing is, we know how to do this!
At MOH we are self-proclaimed neuro-geeks…this is the stuff we do really well and we love doing it.
By understanding the anatomy of the nerve and its related muscles, joints and bones we can identify what biomechanical factors may be contributing to your symptoms. And by having an in-depth knowledge of neurophysiology (nerve function) we can address your sciatica in the way it needs, by treating the nerve itself.
There are a range of manual techniques that can be applied to help reduce the sensitivity of the sciatic nerve. Some of these include gentle hands on treatments like soft tissue massage and joint mobilisations, and even performing mobilisations of the nerve itself. These approaches can help to free up the nerve pathway, improve neural blood supply and fluid flow, restore mobility and decrease sensitivity.
This sort of approach is great for helping to reduce abnormal activity in the nerve and reduce symptoms. It is perfectly complemented by a carefully planned and well calibrated exercise rehabilitation program. This is also extremely effective in improving neuromuscular control and reducing nerve sensitivity.
Lastly, but certainly not least we can help to make changes to the strongest driver of nerve pain…your brain. By helping you to understand the nature of your condition, what makes it better and worse, and why you are still experiencing these symptoms – you can actually turn the volume down on your pain all by yourself… and that is backed by a tonne of research in pain science.
If you are experiencing sciatica and need a helping hand to get back to doing the things you love, make an appointment with one of our Osteopaths, click here.
If you’re not sure if we can help you specifically, please get in touch so we can help put you on the path to recovery, call 03 8370 3044.



